Seoul National University Hospital, Mothers with pre-existing Hypertension and concurreded Preeclampsia Face Threefold Higher Post-Childbirth Cardiovascular Risk
- A follow-up study of 570,000 Korean mothers confirms all five HDP subtypes increase long-term risk of cardiovascular events.
- Mothers with "Superimposed Preeclampsia"—preeclampsia on top of pre-existing hypertension—exhibit the highest risk... Personalized cardiovascular care is essential after delivery.
Research results indicate that hypertension during pregnancy should not be regarded merely as a temporary obstetric complication, but as an important warning sign requiring continuous cardiovascular monitoring even after childbirth. Women who experienced gestational hypertension (HDP) were found to have a significantly higher risk of developing cardiovascular diseases, such as heart failure and stroke, even years after delivery. In particular, mothers who experienced ‘preeclampsia in succession,’ a condition where pre-existing chronic hypertension is superimposed with preeclampsia, had a long-term risk of cardiovascular disease approximately three times higher than mothers without HDP.
A research team led by Professors Jun-Bin Park and Soon-Gu Kwak of the Department of Cardiology at Seoul National University Hospital (including Professor Chan-Soon Park of Asan Medical Center and Professor Kyung-Do Han of Soongsil University) announced the results of a study analyzing the association between gestational hypertension and the long-term risk of cardiovascular disease after childbirth on the 17th . This study was conducted on 570,843 women who gave birth in Korea between 2010 and 2018. The results were published in the latest online edition of JAMA Internal Medicine (IF 23.3), an international academic journal published by the American Medical Association.
Gestational hypertension is a pregnancy complication that occurs in approximately 5–10% of all pregnancies. While the impact of preeclampsia and eclampsia on maternal health is well known, the long-term cardiovascular risks associated with the various subtypes of HDP have not been sufficiently elucidated. To fill this research gap, the research team utilized large-scale domestic data to compare risk levels for each subtype.
The research team categorized HDP into five distinct subtypes for analysis: ▲Chronic hypertension, ▲Gestational hypertension, ▲Preeclampsia/Eclampsia, ▲Superimposed preeclampsia, and ▲Unspecified hypertension. The study then tracked the risk of major adverse cardiovascular events—comprising cardiovascular death, heart failure, myocardial infarction, stroke, and atrial fibrillation. To ensure accuracy, the analysis adjusted for a wide range of variables, including age, obesity, diabetes, dyslipidemia, and chronic kidney disease, as well as income level, residential area, parity, mode of delivery, gestational diabetes, smoking, alcohol consumption, and physical activity.
According to the analysis, 22,876 (4.0%) of the total participants experienced HDP. Among these cases, gestational hypertension was the most frequent at 34.8%, followed by preeclampsia/eclampsia (32.4%), unspecified hypertension (17.7%), chronic hypertension (12.3%), and superimposed preeclampsia (2.8%). The median follow-up period for the study was 6.5 years.
Mothers who experienced gestational hypertension had a 1.62 times higher risk of developing long-term combined cardiovascular disease compared to those who did not. The incidence rate was 4.39 cases versus 2.29 cases per 1,000 person-years. This means that when 1,000 people were followed for one year, there were approximately 2.1 more cases of cardiovascular disease.
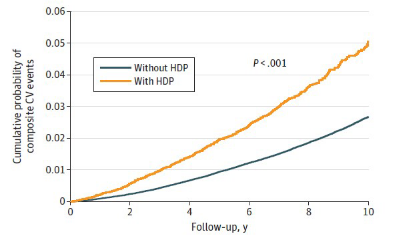
[Graph 1] Mothers who experienced hypertensive disorders of pregnancy (orange line) showed a higher cumulative incidence of major adverse cardiovascular events compared to those who did not (black line), with an adjusted hazard ratio of 1.62.
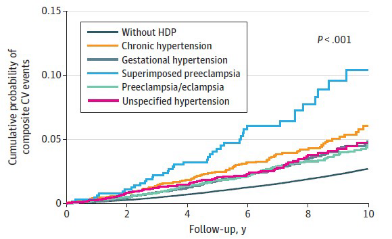
[Graph 2] Among the five subtypes, the cumulative incidence for the superimposed preeclampsia group (light blue line) rose most steeply. This group exhibited the highest risk, with an adjusted hazard ratio of 2.93 compared to mothers who did not experience hypertension during pregnancy.
By subtype, the superimposed preeclampsia group exhibited the highest risk. The adjusted hazard ratio for this group was 2.93, indicating that their risk of long-term cardiovascular disease was approximately three times higher than that of mothers without HDP. This was followed by chronic hypertension (1.81 times), unspecified hypertension (1.61 times), gestational hypertension (1.53 times), and preeclampsia/eclampsia (1.50 times).
When analyzed by specific disease type, the risk of heart failure and stroke was found to increase across all five subtypes of gestational hypertension. Conversely, the risk of myocardial infarction and atrial fibrillation varied depending on the HDP subtype. A significant association for myocardial infarction was observed primarily in the unspecified hypertension group, while an increased risk of atrial fibrillation was identified in both the chronic hypertension and unspecified hypertension groups. These results suggest that HDP is not a single, monolithic disease, but rather that the pattern of future cardiovascular disease risk may vary depending on the specific subtype experienced during pregnancy.
The research team explained that HDP and subsequent cardiovascular diseases may share common underlying mechanisms, such as endothelial dysfunction, chronic inflammation, and metabolic abnormalities. In particular, the study analyzed that superimposed preeclampsia may reflect a more complex and severe clinical state during pregnancy. Consequently, the researchers emphasized the necessity for more meticulous and long-term cardiovascular follow-up for these patients even after childbirth.
Professor Jun-bin Park(Department of Cardiology at Seoul National University Hospital) stated, "Blood pressure issues during pregnancy should not be regarded merely as a temporary phenomenon that disappears with childbirth, but should be recognized as an important signal requiring future cardiovascular health monitoring. In particular, high-risk pregnant women with pre-existing chronic hypertension who also have preeclampsia must actively take steps to prevent cardiovascular disease even after childbirth through regular cardiovascular checkups with a specialist and lifestyle management."
However, the research team noted that as this was a large-scale observational study, it cannot definitively conclude that HDP are the direct cause of subsequent cardiovascular disease. They further added that it is important to consider that the study population was limited to women who had accessible data from national health examinations within two years prior to their pregnancy.

[From left] Professor Soon-gu Kwak and Professor Jun-bin Park, Department of Cardiology, Seoul National University Hospital