Depressed adolescents responding to antidepressant treatment; Nerve cell recovery potential↑
Depressed adolescents responding to antidepressant treatment;
Nerve cell recovery potential↑
- Seoul National University Hospital, to examine neurobiological changes associated with during treatment of adolescent depressive symptoms in the brain
- In the group that responded to antidepressant treatment, dorsolateral prefrontal cortex volumes increased and the possibility of nerve cell recovery is high.
Recently, research has shown that depressed adolescents who respond to antidepressant treatment are more likely to recover atrophied nerve cells and maintain a comfortable brain state. This is expected to provide a new perspective in understanding the mechanism of antidepressant treatment in depressed adolescents.
On August 22nd, Professor Kim Jae-Won's team from the Department of Pediatric Psychiatry at Seoul National University Children's Hospital announced the results of an analysis of neurobiological changes that occur in the brain during antidepressant treatment in 95 depressed adolescents aged 12 to 17.
In general, antidepressants are most frequently prescribed to treat depression in adolescents, and in particular, selective serotonin reuptake inhibitors (SSRIs) are prescribed as the first drug treatment for adolescent depression with moderate or higher levels of symptom severity.
SSRI treatment alone or in conjunction with other treatments, such as cognitive behavioral therapy, showed remission rates of approximately 55% and 60%, respectively, in adolescents.3 Given the relatively insufficient efficacy of SSRIs, increasing treatment efficacy is one of the central issues in treating adolescents with major depressive disorder (MDD). One possible way to improve treatment efficacy is to understand the neurobiological changes related to SSRIs during the course of treatment for depression. Thus, it is important to examine neurobiological treatment markers that are associated with improving depressive symptoms.
However, research on the neurobiological treatment mechanisms of adolescent depression is still insufficient worldwide.
The research team studied 95 depressed adolescents and 57 non-depressed adolescents who visited the ‘Mood and Anxiety of Youth (MAY) Clinic’ at Seoul National University Children’s Hospital from 2015 to 2018 and investigated the effect of selective serotonin reuptake inhibitor treatment on the neurobiological characteristics of the brain in depression.
A depressed adolescent was treated with escitalopram, an antidepressant of the selective serotonin reuptake inhibitor class, for 8 weeks. In this process, the research team used CDRS-R (Children’s Depression Rating Scale-Revised), a depression assessment tool for children and adolescents, to evaluate depressive symptoms before and after treatment. The research team collected structural brain MRI and resting-state functional MRI (rsfMRI) data together.
The research team classified adolescents whose depressive symptoms decreased by more than 40% after treatment compared to before treatment as the treatment responder group and adolescents whose depressive symptoms did not decrease by more than 40% compared to before treatment as the treatment non-responder group. Afterwards, the research team analyzed the correlation between changes in depressive symptoms and changes in the dorsolateral prefrontal cortex (DLPFC) volume and resting-state functional connectivity (rsFC). The dorsolateral prefrontal cortex is one of the major brain regions involved in emotional regulation and cognitive control.
As a result of the analysis, approximately 54% of depressed adolescents were classified into the treatment response group whose depressive symptoms improved after antidepressant treatment, and the dorsolateral prefrontal cortex volume increased in the treatment response group compared to the non-responder group.
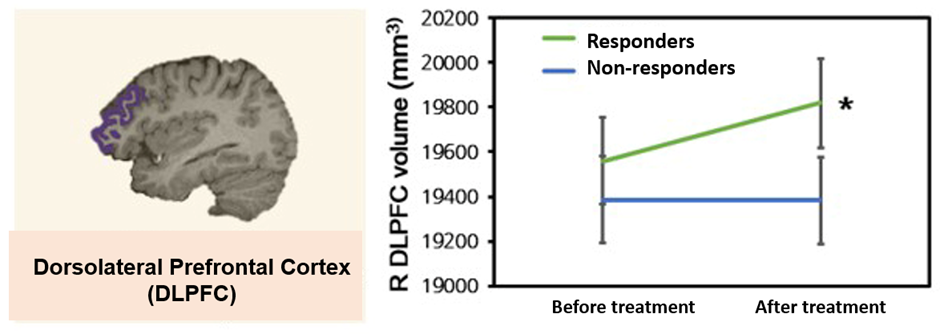
[Figure 1] Changes in dorsolateral prefrontal cortex (DLPFC) Gray Matter Volume before and after antidepressant treatment (R=right, *statistically significant at p<0.05)
It is known that the decrease in prefrontal cortex volume that occurs in depression is related to neural atrophy. ‘The fact that the dorsolateral prefrontal cortex volume increased after antidepressant treatment suggests that it may be related to the recovery of nerve cells that had atrophied due to depression,’ the research team explained.
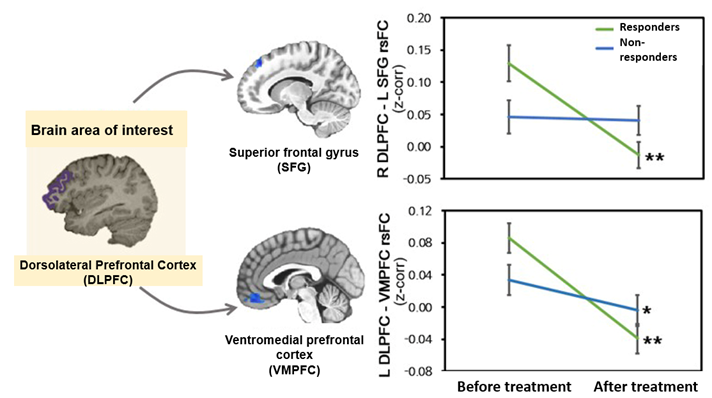
[Figure 2] Changes in resting state functional connectivity of the dorsolateral prefrontal cortex before and after antidepressant treatment (R=right, L=left, *p<0.05, **p<0.01, statistically significant)
Additionally, in the treatment response group, resting functional connectivity between the dorsolateral prefrontal cortex, superior frontal gyrus, and ventromedial prefrontal cortex was found to be decreased. The research team emphasized that the decrease in resting functional connectivity, which refers to a resting state of the brain in which the control of emotions or cognitive functions is not activated, can be interpreted as depressed adolescents showing a more comfortable brain connection state after treatment.
Additionally, the results showed that the more the adolescent's depressive symptoms improved, the more the dorsolateral prefrontal cortex volume increased, and conversely, the more the functional connectivity decreased.
Professor Kim Jae-Won said, “This study is an important result that shows that antidepressant treatment can be accompanied by changes in brain structure and functional connectivity responsible for emotional regulation and cognitive control in adolescent depression.” “We hope that data related to changes in brain structure and functional connectivity can be used as biomarkers for antidepressant treatment in the future.”
This study, which was conducted with support from the National Research Foundation of Korea's mid-career researcher support project, was published in the renowned international academic journal ‘JAMA Network Open (IF=13.8).’