Is Obsessive-Compulsive Disorder (OCD) caused by the cortico-striatal circuit in the brain?
- Seoul National University Hospital identified aberrant cortico-striatal white matter connectivity and associated subregional microstructure of the striatum, a key circuit for OCD
- “Expected to locate an accurate brain region for targeted therapy such as neuromodulation”
The results of a study that brings us one step closer to identifying the cause of obsessive-compulsive disorder (OCD) were published. For the first time, a Korean research team discovered damage to the structure of the 'cerebral cortex-striatal circuit', known as the core brain neural circuit of OCD.
On June 17, research results were published that revealed changes in the white matter connecting the cerebral cortex and the striatum and damage to the microstructure of the striatum using the latest brain images of OCD patients by Professor Kwon Jun Soo's team, Department of Psychiatry, SNUH (Professor Kim Minah, Park Hyungyou, PhD candidate, Department of Brain and Cognitive Science, Seoul National University)
OCD is a prevalent psychiatric disorder characterized by uncontrollable and repetitive intrusive thoughts or images (i.e., obsessions) and repetitive behaviors to cope with anxiety stemming from such intrusive thoughts (i.e., compulsions). There is much evidence that highlights cortico-striatal circuitry as one of the neural bases of OCD.
‘The striatum’ is an important brain region that receives inputs of cortical information and is involved in reward, executive, self-regulatory, and motor processing. Therefore, it has been suggested that the damaged neural function of the neurocircuit in cortico-striatal circuitry is a cause of OCD.
However, the abnormal white matter connectivity and abnormal mechanisms of the associated subregional microstructure of the striatum that cause the imbalanced function of the cerebral cortex-striatal circuit had not been investigated so far.
The research team focused on the cortico-striatal white matter connectivity in OCD patients. The brain white matter circuit connecting the cerebral cortex and the striatum was reproduced using MRI diffusion tensor imaging (DTI) of 107 non-medicated OCD patients and 110 healthy controls. Afterwards, the white matter connectivity of each circuit was compared and analyzed.
They identified significantly reduced orbitofrontal WM connectivity with its associated striatal subregion in patients with OCD compared to that in HCs. However, OCD patients exhibited significantly increased caudal-motor and parietal connectivity with the associated striatal subregions.
In other words, it was confirmed that the balance of the cerebral cortex-striatal circuit was disturbed in the case of OCD patients. Our results highlighted contrasting patterns of striatal WM connections with the orbitofrontal and caudal-motor/parietal cortices, thus supporting the cortico-striatal circuitry imbalance model of OCD.
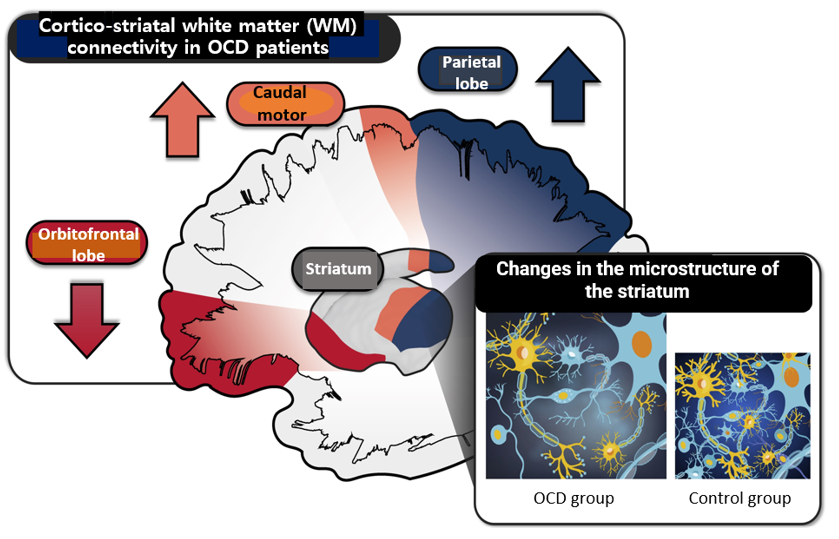
[Image] Changes in the cortico-striatal circuit observed in OCD patients. While connectivity with the orbitofrontal cortex decreased, connectivity between the motor cortex and the parietal lobe increased, indicating that the cortex-striatal circuit was out of balance. In addition, the research team confirmed that the microstructure of the striatal region was also damaged in OCD patients.
It was also found that the microstructure of the striatum connected to the motor cortex and parietal lobe diminished in patients with OCD as a result of observing changes in the striatal microstructure using diffuse kurtosis imaging (DKI). This means that nerve cells or tissues in the striatal region of the OCD group were damaged compared to the general population.
The research team emphasized that this study is the first to identify aberrant cortex-striatal white matter connectivity and microstructural changes in the striatal subregion of obsessive-compulsive disorder (OCD) patients.
Professor Kim Minah and Park Hyungyou, a PhD candidate, said, “We have identified the structure of the neural circuits that are out of balance in OCD patients by comprehensively observing abnormalities in the white matter connecting the cerebral cortex and the striatum and damage to the microstructure of the striatum.” "This could contribute to understanding the structural mechanisms of brain neural circuit abnormalities in OCD," they said.
Professor Kwon Jun Soo said, "This study contains important results proving the neural mechanism proposed as a hypothesis in the study of OCD." He also expected that “these findings will be used to present an accurate target area for treatment such as neuromodulation to directly stimulates the brain of OCD patients.”
This study was published in the latest issue of the international SCI journal ‘Molecular Psychiatry (IF=15.99)’.

[Picture from left] Prof Kwon Jun Soo andProf Kim Minah of Department of Neuropsychiatry at SNUH, and Park Hyungyou of Department of Brain and Cognitive Sciences at SNU