In the case of a medical history of Allergic-like Hypersensitivity Reactions(HSR) to CT contrast agents, the HSR risk for MRI may increase
- Seoul National University Hospital reveals association between hypersensitivity reactions to MRI and CT contrast agents
- To reduce the risk of HSR, it is necessary to check the patient's previous medical history of contrast agent
It was found that hypersensitivity reactions to MRI and CT contrast agents, which had previously been considered separate problems, are actually related. A previous medical history of HSRs to one of the MRI and CT contrast agents is associated with a significantly higher risk of HSRs to the other, a new study found. This is the first time this has been confirmed internationally and it is attracting academic attention.
On March 4, Professor Kang Hye-Ryun's team at Seoul National University Hospital's Drug Safety Center published the results of a study: a cohort analysis on the association between hypersensitivity reactions (HSRs) to two contrast agents on 154,539 patients who used MRI contrast agents and 261,426 patients who used CT contrast agents over 8 years from 2012 to 2020.
Contrast agents are drugs that are administered to the human body so that specific tissues or blood vessels can be seen clearly in imaging tests, but they also have side effects. In particular, HSRs may cause allergy-like symptoms such as rash and flushing.
Gadolinium-based contrast agent (GBCA) is used for MRI and Iodinated contrast media (ICM) is used for CT. Since each contrast agent has completely different component structures and chemical properties, HSRs caused by the two contrast agents have been considered to be independent of each other.
However, in actual clinical practice, some patients showed HSRs to both contrast agents, so additional research was needed on the correlation between MRI and CT contrast agents to enable safer use of contrast agents.
As a result of the study, the prevalence of HSRs to MRI and CT contrast agents was 0.7% and 3%, respectively, and fewer patients experienced HSRs to MRI contrast agents. That is, the risk of HSR was relatively low for MRI contrast agents compared to CT contrast agents.
To determine the correlation between MRI and CT contrast agent HSR, the research team performed a detailed analysis only on patients who had used the other contrast agent in the past.
The prevalence of MRI contrast agent HSR in patients who had experienced and had not experienced CT contrast agent HSR in the past was respectively 3% and 0.7%. In addition, the prevalence of CT contrast agent HSR was respectively 15% and 4% in patients who had and did not have experience of MRI contrast agent HSR in the past.
In other words, the risk of HSR increased by 4 times when using the other type of contrast agent if there was a history of HSR with MRI or CT contrast agent.
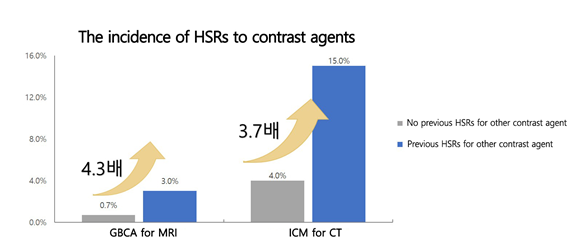
[Figure.1] Patients with a history of HSR to one of the MRI or CT contrast agents are approximately 4 times more likely to develop HSRs when using the other contrast agent.
An additional analysis was conducted to effectively prevent recurrence of HSRs to contrast agents. In the meantime, antihistamines or steroids have been administered as a precautionary measure to prevent HSRs to MRI contrast agents. However, it was not clear evidence whether the preventive effect of this measure was sufficient.
As a result of the analysis, the average recurrence rate was 15% when a patient who had experienced an MRI contrast agent HSR used the MRI contrast agent again. The recurrence rate was reduced from 20% to 14% with prior administration of antihistamines or steroids compared to without them.
However, when the contrast agent that caused the hypersensitivity reaction was changed, the recurrence rate of a HSR decreased from 21% to 5% compared to the cases without changing the agent. This was found to be more effective in preventing recurrence. When prophylactic drug administration and contrast agent change were combined, the recurrence rate could be reduced from 31% to 5% compared to the cases without any pretreatments.
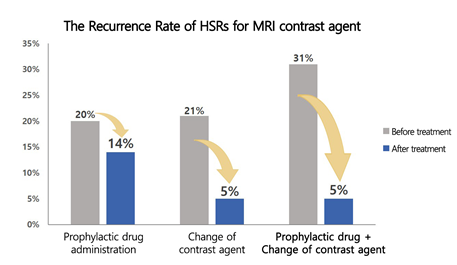
[Figure2] When the HSR contrast agent was changed, the recurrence rate was reduced to 1/4 of that before treatment, which was more effective in preventing recurrence than administering a prophylactic drug. When prophylactic drug administration and contrast agent change were combined, the HSR recurrence rate was reduced to 1/6 the level before treatment.
This study confirmed the fact that HSR to MRI and CT contrast agents, which were previously considered separately, increased the likelihood of each other. In addition, the research team emphasized that it is of great clinical significance in that it was the first in the world to suggest the need to check medical records for HSRs to contrast agents in the clinical field.
Professor Kang Hye-Ryun (Dept. of Allergy, Internal Medicine), Director of the Drug Safety Center, said, “The contrast medium is essential for an accurate test." and "In order to minimize the risk of hypersensitivity reactions, it is necessary to prepare a history of contrast agent use so that information on contrast agents used in the past can be confirmed,".
She added, “If a hypersensitivity reaction occurs, detailed information such as the name and ingredients of the contrast agent should be shared with the patient so that they can safely use a contrast agent even if they go to another medical institution in the future.”
This research was published online in the latest issue of Radiology, an international radiology journal.

[Pictures, from left] Prof Kang Hye-Ryun (Dept of Allergy, Internal Medicine), Dr Ahn Yoon Hae (Internal Medicine Clinical Fellow, 1st Author), Prof Kang Dong Yoon (Drug Safety Monitoring Center, 1st author)