Development of angiogenesis-blocking anticancer drugs that inhibit cancer growth/metastasis
- Promising future platform of new biotherapeutics development for cancer or vascular retinopathy based on angiogenesis-blocking effect
A Korean research team discovered a key gene that inhibits angiogenesis and thus, using it, started developing an anticancer drug that suppresses cancer metastasis.
This research, led by Seoul National University Hospital Professors Kim Hyo-Soo and Kwon Yoo-Wook, was published in the Journal of Hematology & Oncology (IF; 17.4), a world-renowned journal in the field of foundational cancer research.
Angiogenesis is a process in which new blood vessels are created from existing blood vessel structures and is regulated by the interaction between endothelial cells and surrounding pericytes. While the role of vascular endothelial cells has been widely studied worldwide up until now, research on pericytes has been insufficient. Inhibiting angiogenesis can prevent cancer growth.
Professor Kim Hyo-Soo's team discovered that the KAI-1 (KAI1/CD82) gene was expressed in pericytes. For the first time in the world, they found that KAI-1 plays an important regulator role in inhibiting angiogenesis and maintaining vascular homeostasis.
The KAI-1 protein synthesized in pericytes increases the expression of the angiogenesis inhibitory factor LIF after it settles on the cell surface. In addition, KAI-1 inhibits angiogenesis by binding to VEGF or PDGF, the representative cytokines that induce angiogenesis, and blocking their receptors’ binding function.
The research team used the angiogenesis inhibitory effect of the KAI-1 protein to develop a new cancer treatment. The KAI-1 peptide was prepared by analyzing the molecular structure and amino acid sequence of the site where KAI-1 binds to the angiogenesis cytokines VEGF and PDGF. They also created a tumor model by transplanting breast and prostate cancer cells into mice. The tumors were nourished by the formation of numerous blood vessels and gradually increased in size. When the KAI-1 peptide was administered, the tumor size was dramatically reduced by inhibiting angiogenesis.
In addition, the research team found that pericytes exist around endothelial cells constituting mouse retinal blood vessels and that the KAI-1 protein is mainly expressed in pericytes, not vascular endothelial cells. Thus, it was revealed that the mouse retina in which KAI-1 was removed through genetic manipulation had much more active blood vessel formation.
In an animal model of diabetic retinopathy, when the KAI-1 peptide was administered, it suppressed angiogenesis and showed a therapeutic effect of suppressing retinal blood vessel hyperproliferation to a level similar to that of normal standards.
The KAI-1 peptide can inhibit tumor growth and prevent cancer metastasis by inhibiting angiogenesis, so it is expected to improve patients’ results when used in combination therapy with existing anticancer drugs. It can also be used as a treatment for diseases caused by hypervascularization, such as diabetic retinopathy.
Since 2016, the research team devoted themselves to this study after announcing to the world that the KAI gene is the key to the immortal mechanism of bone marrow hematopoietic stem cells.
Professor Kim Hyo-Soo, who directed this project for five years, said, “With the hard work of various members of the center of CBT(Cell and Bio Therapy for heart, diabets & cancer), great results have been achieved. In the future, we plan to pursue advanced work to develop the KAI-1 peptide as a bio-therapeutic agent for anticancer and vascular retinopathy.”
Meanwhile, this project was carried out as part of the work being done at the center of CBT, which is supported by the Ministry of Health and Welfare, and research-oriented hospital.
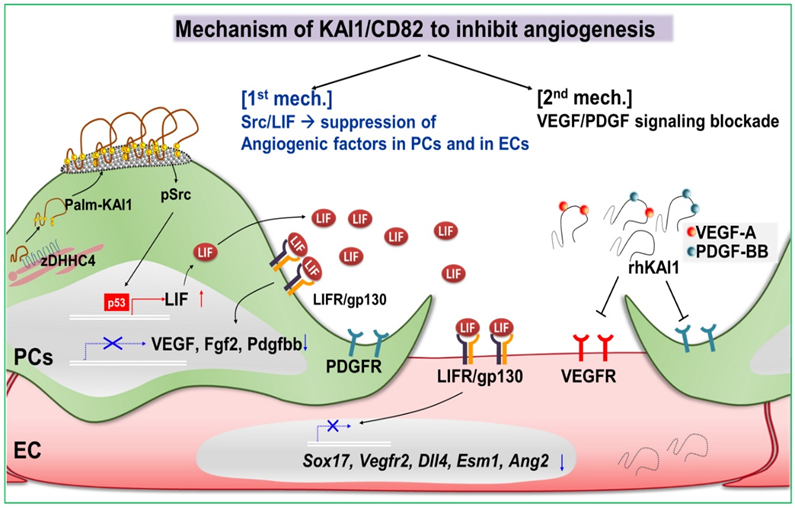
[Figure 1] Mechanism of KAI1/CD82 to inhibit angiogenesis
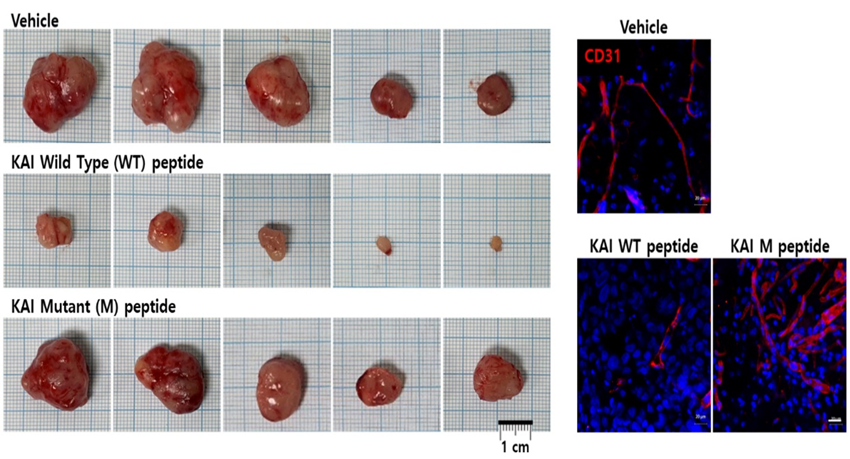
[Figure 2] Anticancer effect of KAI-1 peptide in a mouse tumor model. Treatment with KAI peptide may inhibit tumor angiogenesis and reduce the size of cancer. The control group, the mutated peptide, had no therapeutic effect on outcomes.
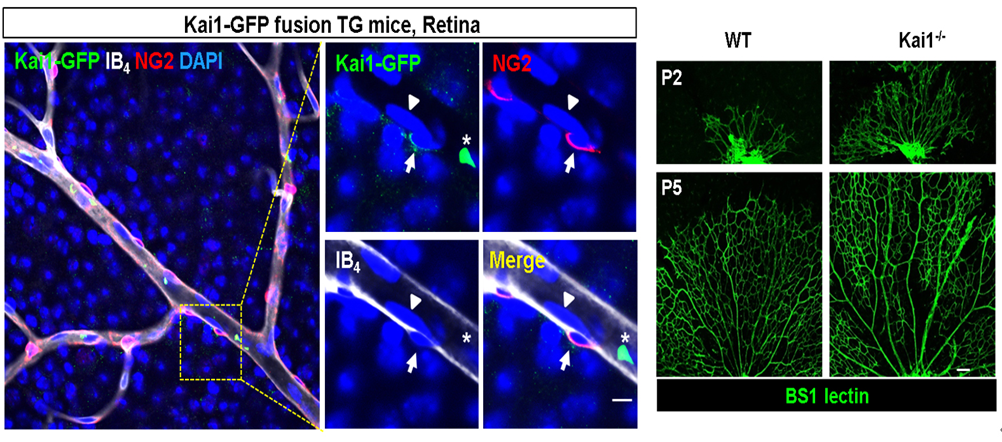
[Figure 3] KAI-1 expressed in pericytes located around blood vessels in the mouse retina. As shown in the picture on the right, when the KAI gene is knocked out, retinal blood vessels show overgrowth.
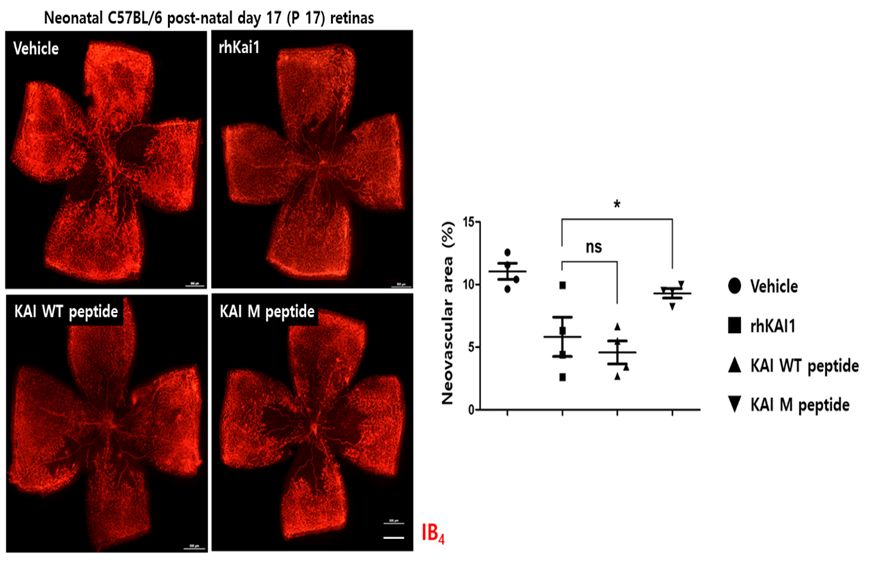
[Figure 4] Confirmation of therapeutic effect on diabetic retinopathy using KAI-1 peptide. Treatment with KAI-protein or KAI-peptide can inhibit retinal blood vessel hyperproliferation.

[Photo] Left: Prof Kim Hyo-Soo; right: Prof Kwon Yoo-Wook